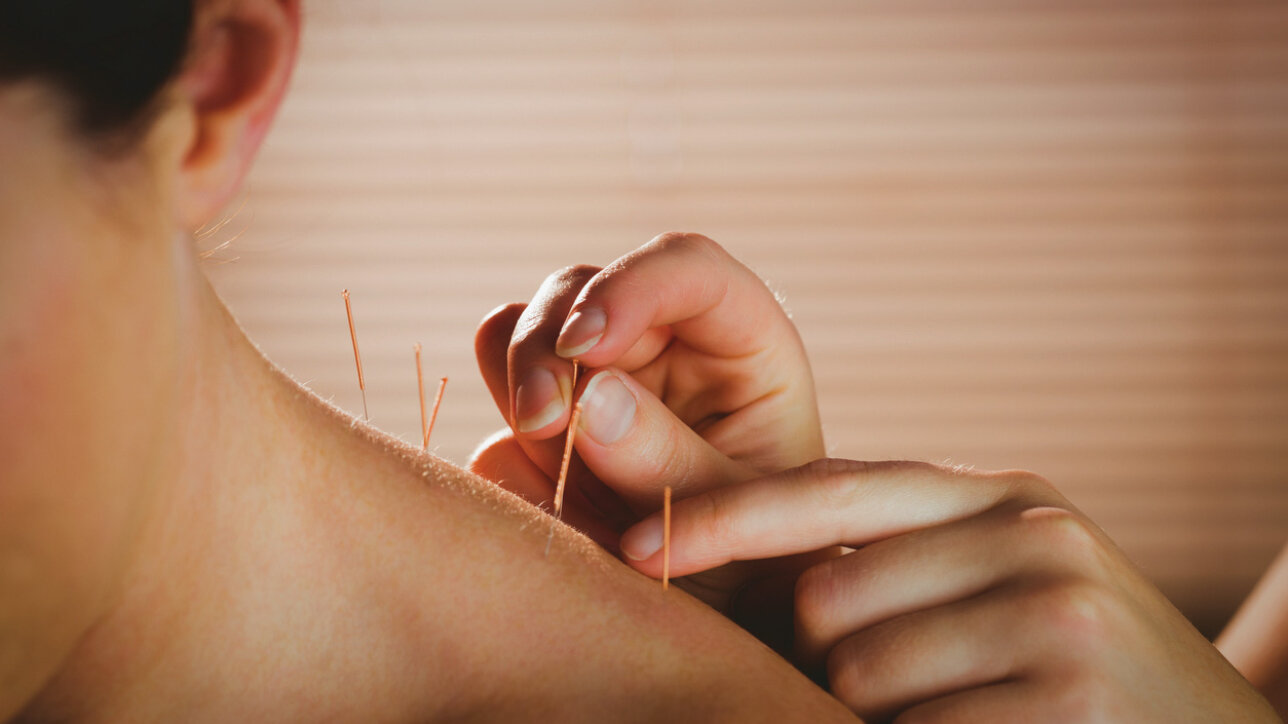
Dry needling – What’s the point?
The first question usually asked is: What is it?
By definition, dry needling is a skilled technique performed by a physical therapist using filiform needles to penetrate the skin and/or underlying tissues to affect change in body structures and functions for the evaluation and management of neuromusculoskeletal conditions, pain, movement impairments, and disability.
So, what exactly does that mean?
Dry needling uses very small monofilament needles that are “dry” meaning there is no medicine in or on the needle. In contrast, a “wet” needle typically refers to a hypodermic needle used for injections, which are much larger than those used for dry needling. Dry needling involves inserting needles into sub-dermal structures such as muscles, tendons, ligaments, bone, scar tissue, peripheral nerves, and neurovascular structures to elicit a local and systemic response, aiding in pain reduction and improved movement patterns.
Is it safe?
Dry needling is very safe; serious side effects can occur in less than 1 treatment per 10,000 (less than 0.01%). The most serious side effect from this, is pneumothorax (lung collapse due to air inside the chest wall). Other minor side effects include drowsiness, tiredness, dizziness, minor bleeding or bruising.
Does it hurt?
No, in general dry needling does not hurt. Some areas can bemore sensitive than others, but generally, after the initial needle insertion the needles are no longer felt. At times a deep ache is felt when the needle is inserted and while it is in place for the treatment.
What is the process?
There are different dry needling techniques that your therapist may use. One technique uses a quick in and out method with the goal of eliciting a twitch response from the tight muscle tissues. This technique will cause increased blood flow to the area. This increase in blood flow brings oxygen to the area of muscle holding, allowing the muscle to return to a more relaxed state3.
Another technique targets areas of teno-osseus junctions (where tendons attach to bone). This technique referred to as pecking uses the needle to tap around the insertion point of the tendon on a bony surface to break up adhesions or scarring and generate increased blood flow.
Researchers have established protocols for placing needles in non-trigger point targeted areas (muscles, tendons, ligaments, or neurovascular structures) as the third technique. The needles remain in place for 10-30 minutes and are either manually turned periodically throughout the treatment time or connected to a machine that provides electric stimulation. The electro-dry needling technique yields the best analgesic effects. The electric current stimulates a better response by activation of more pain inhibiting centers in the brain, as well as activating local changes in the muscles.
Who benefits from Dry Needling?
Dry needling is a modern, science-based intervention for the treatment of pain and dysfunction in musculoskeletal conditions such as:
- Neck pain
- Shoulder impingement
- Tennis elbow
- Neck pain
- Knee pain
- Shin splints
- Plantar fasciitis
- Back pain
Dry needling has also been found to be beneficial for:
- Arthritis
- Carpal tunnel syndrome
- Headaches
- TMJ disorders
- Radiculopathies
- Chronic pain
- Sciatica
- Fibromyalgia